“Your husband’s blood oxygen has dropped. It’s hovering around 47% right now. Below 50% we usually see brain damage.”
The words hit me like a rock against my skull. All of us went so silent that the quiet crushed against my eardrums.
“Is my husband going to live?”
Those were words I never expected to hear coming out of my mouth at this point in life. Especially given Ed was only 47.
The doctor hesitated.
But I was blunt, direct, to-the-point, with words that meant I wanted no fluff answers. I had been in the medical field too long. I knew how doctors and nurses sometimes sugar-coated things or used evasive words so as not “freak the family out.” I didn’t want coddling or patronizing. I couldn’t bear “uncertainty.” Tell me now – Is he dying or is he going to make it?”
Even though Ed had just been admitted to the ICU from the ER, I thought we had a chance. They had finally diagnosed him in the ER as having severe hyponatremia — blood sodium so low it almost killed him. But they said they could treat him. So what had changed?
The doctor took a breath. My mind rapidly assessed his face, calculated in his delay in answering, and knew before he spoke his most carefully chosen words, that we were dealing with yet another descent toward Ed’s death.
“Your husband is young and strong…” was all he said.
That trip
I always struggled anytime Ed traveled on business. Struggled was an understatement. Phobic that something would happen to him is more accurate. I knew from the time my aunt was killed in a car accident when I was 9, that phone calls can come and inform you that the “thing that usually doesn’t happen,” just did. I never forgot my mom’s intense wail when she heard her sister was dead.
So, I held that same fear again in early 2005, when he had to travel with a few guys from his office to a meeting in New York City. And it was with that same huge sigh of relief I always felt on his return that I picked him up from the airport. It always felt like we’d been given yet another “reprieve,” until the next time.
And even though he looked exhausted and had caught some bug, at least he was back. The rest we could deal with.
For the rest of the year, though, and all through 2006, he had a constant sinus infection. All the usual things – nasal saline, nasal steroid sprays, antibiotics – wouldn’t touch it.
Finally, out of desperation, we went to an ENT. He, too, prescribed another round of nasal steroid spray. Then, when that didn’t work, he gave Ed a round of oral prednisone. Which should have worked…but it didn’t.
So the doctor moved up to his big guns: a very-high-dose, month-long round of steroids. Failure again.
At that point, the doctor ordered CT scans of the skull. To this day, I absolutely HATE those large sheets with cross-section images of Ed’s skull. Because there in THAT image was something we couldn’t ignore – the “unilateral mass.”
That basically meant that there was “something there,” only on one side. Who knew what that something was? It could have been the cause of his problems or not. And it could have been anything from nothing at all to cancer. So, we couldn’t ignore it.
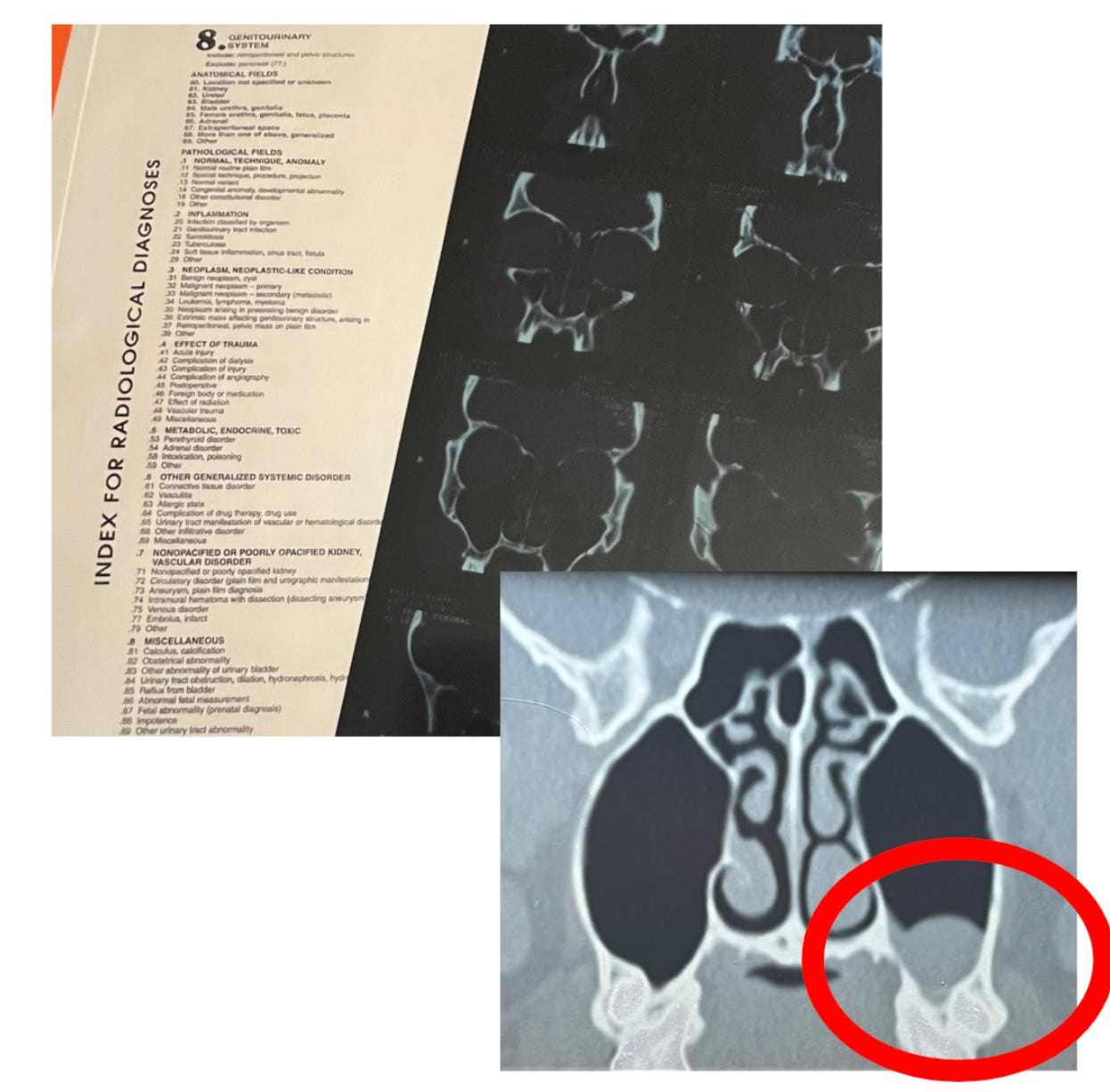
If there is anything I am even more phobic about, even worse than business trips, it’s me or anyone I love having to undergo any kind of surgical procedure. You would think I would be fine with that after 30 years in the medical field. But I’d seen too many things over those years. I didn’t want to be anywhere near a hospital, and I didn’t want anyone I loved near a hospital.
So every time I held that X-ray film up to the window and studied that image, I felt a hatred for that mass, and a sense of foreboding.
But knowing that my phobias, though understandable, could not run my life, I sucked it up and put on a brave face. When we got to the day-surgery center, I reminded myself that thousands of people have procedures every day and “things usually don’t happen.”
Yes, I grilled the condescending anesthesiologist about exactly what chemical they were giving him for anesthesia. Yes. I asked about his lab results that they did. Yes, I was terrified when they wheeled him away. But as I sipped tea in the waiting room, I convinced myself that my fears were overblown. Everyone else sitting there was reading a magazine, chatting on the phone, or looking generally bored. So, I told myself to just trust that all would be well.
And when they called me into the recovery room, he sat there, smiling, sipping soda, and chatting away. He seemed to have shrugged off the anesthesia well. And even though the surgeon had to operate in an area just a couple of millimeters under his brain…under his pituitary gland to be specific, all had apparently gone off without a hitch.
They told me what pain meds to give and when, how to take care of the wound dressing, and change it. We settled in at home for a quiet evening that should have seen Ed sleep off the rest of the anesthesia and pain meds, and wake up refreshed and alert in the morning.
Should have.
Just let him sleep it off!
The afternoon went sort of okay. He slept. But he kept wanting more water to drink. Seemed to be very thirsty. And he was acting off, not really with it. While I couldn’t put my finger on it, things just felt “wrong.” He’d had previous pain meds after dental procedures and had not reacted like this.
Trusting my gut, I called the surgeon and told him what I saw. The surgeon snapped at me. “He’s just out of it from the pain meds! Let him sleep it off!”
I was in a quandary. I knew Ed. Things seemed off. But I also knew I was nervous, so…I believed the doctor.
Just have them catheterize him!
The next day, I sent our son off to school. Ed got up, but was distant. Strange. Quiet. He seemed detached from things around him. But he answered me. Sort of.
But he couldn’t zip his pants. His abdomen seemed swollen. His feet, too, wouldn’t fit in his loafers. I called the doctor’s office. The equally abrupt nurse blew me off.
“He’s retaining fluid! Something is wrong.”
“Just take him to the ER then and have them catheterize him!” I don’t think she was listening to me.
“I didn’t say he couldn’t go to the bathroom! I said he is RETAINING FLUID! He is SWELLING all over his body!”
“Then take him to the ER.” She clearly just wanted me off the phone.
It was time to get our son from school.
“You’re coming with me,” I said to Ed. I had decided that we might need to get him checked by somebody.
“Do you want to go and get checked at the Urgent Care?”
He mumbled something unintelligible. I didn’t wait for his answer.
The moment our son got in the car, I said to Ed again, “We can go to the Urgent Care or the ER.”
He just stared at me and couldn’t answer. I went right to the ER.
What is this?
It was blessedly quiet there, a rare occurrence. They took him right back, and the nurse started to ask him some of the usual intake questions. He couldn’t answer. Then she did something that flooded me with terror.
“What is this?” she asked Ed. She was pointing at his watch.
Ed sat there, and I could see him concentrating mightily. Then he looked up at her helplessly, tried to say something, but couldn’t make sense
I thought, My God, he’s having a stroke.
She obviously thought so too, because she immediately admitted him into the ER, did all the vitals, and then sent him for a CT scan of his brain. I waited.
They wheeled him back a short time later. He was no longer conscious.
I sat quietly near him. Waiting for the results. That’s when all hell broke loose.
The bag of sneakers
In a matter of seconds, his eyes flipped wide open, and he looked at me like he was angry. His arm shot out hard in my direction like he was throwing a punch. His surgical site in the nose tore open, and blood was everywhere…including down into his lungs.
I thought, *He just aspirated blood into his lungs! He’s a dead man!* I knew from years in the bacteriology lab that when something like that happened, it meant you were at risk of a serious infection as well as damage from fluids going into the lungs that weren’t supposed to be there.
I yelled for the doctors, and though they told me to calm down, they were clearly in emergency mode.
First, they intubated him to get air in his lungs. They started administering meds and performing assessments to figure out what had happened.
I was off to the side. My entire body was shaking. My teeth gritted.
The doctor started firing questions at me: “What meds was he on? What had he been doing today? What was his surgery for? What’s his medical history? Diet?”
As fast as he asked, I answered. Despite the fact that my heart was pounding and I was barely staving off total panic, I knew in that moment that the only way I could help save my husband was to get a grip, think clearly, and answer every question. And…I did.
In between questions, I was saying as many Hail Mary prayers as I could as fast as I could, as well as flat-out pleading with God, and doing deep breathing to stay in control.
I watched as if things were in slow motion. The doctor pricked Ed’s bare foot. Ed didn’t react. I froze and knew what that meant.
The doctor turned to me and voiced the words I was thinking: “I think he’s had a major stroke.”
The room went quiet as they kept working on him. I never left the room. I was frantic, terrified, but in control. I wasn’t leaving him. That’s when the nurse walked in with lab results.
The doctor almost smiled with joy. “He didn’t have a stroke! He’s got severe hyponatremia!” He explained that they actually had something they could work with. They could turn this around, and he would probably be okay. But they had to give the sodium IV VERY slowly. If they gave it too fast and his sodium rose too fast, he could end up paralyzed.
My heart pounded, partly with relief, partly with terror over the risks. But at least we had a chance.
Things calmed for the moment. They brought me papers to sign. My hand shook so hard I could barely hold the pen, much less sign my name.
I heard later that the surgeon came by and they told him what was going on. He never came by to see me. I never spoke to him again. I should have sued him. But at that moment, and for the next many years, I would be too busy to deal with a lawsuit I couldn’t afford anyway. I just cursed the fact that I had EVER listened to him and didn’t bring Ed to the ER that night. I felt responsible for this.
I spoke to my teenage son and told him what was going on. Then I instructed him on how we were going to manage this. I said that “even unconscious people may hear you. I understand that you’ll need to cry. But you do that outside his room. When you go in to see him, you speak strongly, positively, and tell him you are there and love him. Do not cry when you are with him.”
I was shaking all over. Operating on years of hospital training and adrenaline. And the knowledge that we needed to keep under control to be there for Ed. And I needed to be there for my son. So, be strong.
Yet, in that moment, that lifetime of “STRONG” was starting to break apart. All my life, I just bulled through. I had gotten to the point where I didn’t need anybody. Didn’t want to be let down by someone again. So I just took care of things myself. But in these few minutes, everything had changed. I suddenly realized – What do I do if he dies? And I am alone? Who would actually be there for me? Maybe I can’t do it all?
My son and I decided to make a few calls. To a couple of old friends…even though we were no longer that close, I knew they would come. And to one of my siblings, even though she and I hadn’t been on good terms. To neighbors, who could look after our house. To friends of my son. And to my parents, who said they would pray.
At that moment, the doctor came and said Ed needed an MRI to see how his brain was doing. But they were going to have to fight to get him in the machine and would need several techs to help. Because he was on a ventilator, they would have to manually pump oxygen into his lungs when doing the MRI. So it would take a few minutes.
While they arranged everything, I sat there in the now darkened room. Ed was motionless, now changed into hospital garb, and hooked up to all kinds of monitors. His chest rose and fell with the ventilator. The room was silent except for heartbeats, the ventilator, and the beeps of oxygen level numbers up on the screen.
The nurse tapped my shoulder, then gently handed me a plastic bag, and then walked to the desk. I looked down. His sneakers and clothes.
I clutched the bag in shaky hands and thought to myself, Is this how it ends…a bag of sneakers?
To the ICU
People did come. A friend brought us sandwiches. Another friend sat with my son. A neighbor brought blankets and a pillow.
And the many techs were beyond angels. They heard what was happening. Several stayed late and volunteered to work together as a team. Rallied and got him into the MRI machine and kept his oxygen going, tag-teaming with each other to keep pumping the oxygen bag. God bless each one of them.
I watched it all through a small square window in the door to that room. I wouldn’t leave. I couldn’t eat. I needed to know he would survive the MRI.
Finally, they finished. He had cerebral edema – his brain was swelling with fluid against the skull. They would have to monitor him to make sure he didn’t incur any brain damage. It would be a long night. But if they could get his sodium slowly back up, he should make it.
So it was with that hope that I went up to the ICU waiting room with my son and our group of friends to wait while they moved Ed up there. They said they would let me see him when he was all settled.
And that’s when the pulmonary doctor stepped in to tell us about the low blood oxygen level, and hesitated when I asked, “Will my husband live?”
Leave a comment